
Getty Images
Tech issues keep mobile telehealth from reaching underserved
Mobile devices provide a key way to connect underserved patients to telehealth services, but complexity and connection problems keep patients from reaping the benefits.
Video conferencing providers must address technical obstacles that prevent patients -- especially those in underserved groups -- from accessing telehealth on their mobile devices.
Telehealth exploded during COVID-19. Google reported this week that 90% of physicians use telehealth services, compared to just 32% before the pandemic. Virtual visit providers like Zoom and Amwell accommodated this growth, keeping doctors in contact with their patients at a time when physical meetings were restricted.
Smartphones are a key means of accessing telehealth services. A 2020 Doximity survey of more than 2,000 U.S. patients found that 45% wanted to use their cell phones for telehealth visits, while 39% favored laptops. Aaron Miri, CIO of Dell Medical School and UT Health Austin in Texas, witnessed that preference first-hand. He said mobile devices are the predominant way patients connect to video meetings with UT Health professionals.
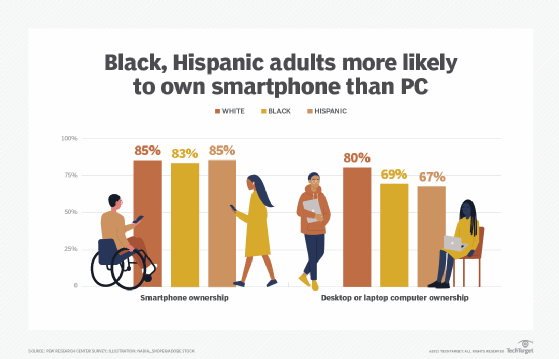
The ubiquity of smartphones means that most people in the U.S. have the technology to participate in a telehealth appointment with their doctors; Pew Research reported that 85% of Americans own a smartphone. Smartphones are the video-conferencing tool most accessible by minority populations. According to Pew, 83% of Black adults and 85% of Hispanic adults own a smartphone, while PC ownership among those groups is 69% and 67%, respectively.
Yet many patients -- including members of underserved groups -- can't reap the benefits of video appointments. A study published by the Institute of Healthcare Policy & Innovation at the University of Michigan in July found that older patients, Black patients and patients in need of an interpreter were among the least-likely groups to use video for their remote visits, opting for audio-only instead. Internet connectivity and technical complexity contribute to this issue.
The COVID-19 pandemic had revealed an "amazing" number of people without internet connections, Miri said. Even in the large city of Austin, schools had to equip buses with Wi-Fi and drive them into neighborhoods so students could learn remotely. Those students -- and their families -- need access to health services as well, Miri said.
Many of those patients prefer telehealth. While they could walk into a hospital or doctor's office, they instead opt to park outside of a Starbucks and use public Wi-Fi on their phones to meet with their doctor virtually, Miri said.
Complexity is another problem. More than half of the 4,302 telehealth users surveyed in a 2020 study by J.D. Power said they had encountered barriers that made it difficult to use telehealth, and 17% of those patients said confusing technology requirements were a hurdle for them. A University of Michigan survey of 1,040 clinicians found nearly 27% felt they needed to provide additional support to patients as they log in and start video visits.
 Aaron Miri
Aaron Miri
"In general, health technology literacy in the general public is low, because people are so used to going into a hospital or going to see [their] doctor," Miri said. "Now, it's almost a requirement of the call centers [for] healthcare providers to have some 'training' for your patients."
Zoom recently released a feature to make it easier for patients to join appointments in the Zoom for Healthcare platform on mobile devices. The feature -- now in beta on Apple iOS -- lets patients join appointments through their mobile browsers. This is intended to save time for healthcare providers, as they no longer have to walk patients through downloading the app.
"Telehealth is ... being used by people of all different demographics, many of whom would not know how to -- or would not want to -- download [an app]," said Zeus Kerravala, principal analyst of ZK Research.
The browser feature will be generally available soon and will come to other mobile OSes, Zoom said.
Miri would like telehealth technology companies to do more to address complexity. For example, Zoom could open a call center to help patients deal with telehealth issues, instead of relying on healthcare providers to provide technical support.
"That would alleviate a lot of burden on the hospitals," he said.
Mike Gleason is a reporter covering unified communications and collaboration tools. He previously covered communities in the MetroWest region of Massachusetts for the Milford Daily News, Walpole Times, Sharon Advocate and Medfield Press. He has also worked for newspapers in central Massachusetts and southwestern Vermont and served as a local editor for Patch. He can be found on Twitter at @MGleason_TT.





